Show summary Hide summary
- How combined sleep disorders reshape cardiovascular risk
- What the veteran study actually found about heart disease
- Turning sleep into a strategic tool against chronic disease
- Practical steps to lower sleep‑related cardiovascular risk
- How do I know if I have both insomnia and sleep apnea?
- Does treating sleep apnea alone reduce heart disease risk enough?
- Can lifestyle changes fix COMISA without medical help?
- Are younger adults really at risk from combined sleep disorders?
- How fast can heart health improve after treating sleep problems?
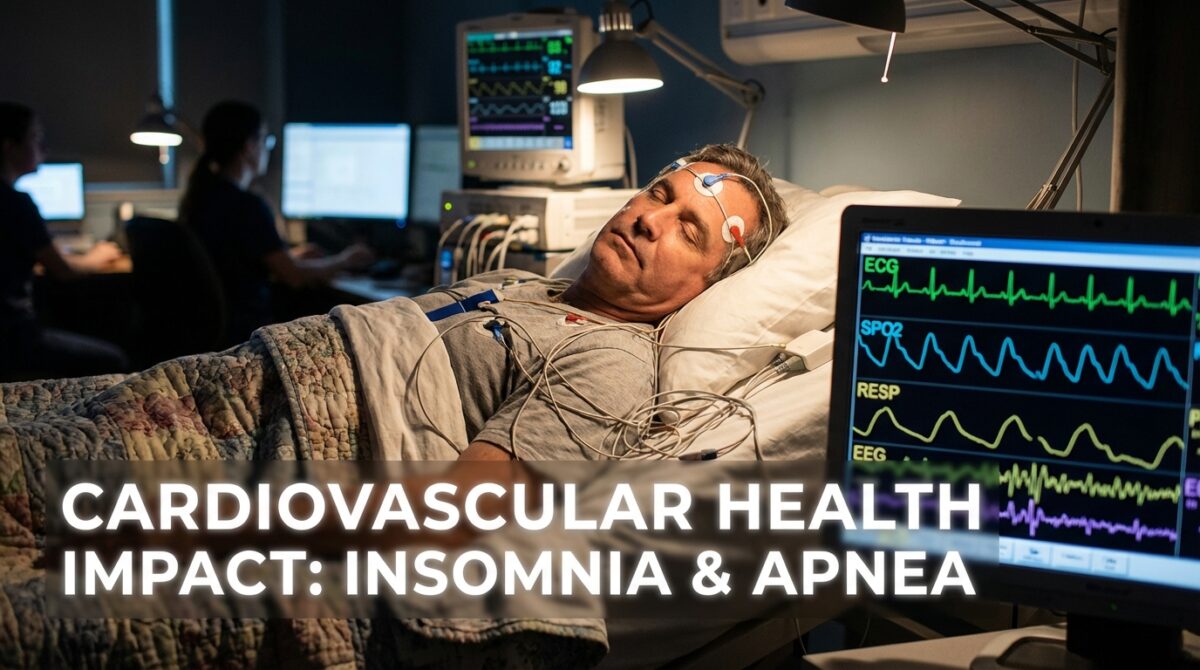
You sleep badly, you snore, you wake up exhausted… and your doctor only checks your blood pressure. Yet a new study on nearly one million veterans shows that the combined impact insomnia and Sleep Apnea can quietly push you toward Heart Disease far earlier than you think.
Researchers from Yale School of Medicine have put numbers on what many cardiologists suspected already: certain Sleep Disorders can act as powerful accelerators of Cardiovascular Risk. When trouble falling or staying asleep meets pauses in breathing overnight, the Health Impact is not just additive, it becomes a dangerous combo that reshapes long-term heart outcomes.
How combined sleep disorders reshape cardiovascular risk
The Yale team focused on post‑9/11 U.S. veterans who underwent testing for Sleep Apnea. Within this huge cohort, they compared adults with insomnia alone, apnea alone, and especially those with both conditions, often called COMISA (comorbid insomnia and sleep apnea). The data showed a markedly higher rate of hypertension and Heart Disease events in the COMISA group.
Unveiling the Secrets of Aging: Mapping 7 Million Cells Across 21 Human Organs
Scientists Unveil a Bacterial Kill Switch That Could Revolutionize the Battle Against Superbugs
This pattern aligns with other large observational work, such as the evidence review on veterans and cardiovascular disease. When repeated arousals from insomnia are layered on top of oxygen drops from apnea, blood vessels face more nightly stress, and early damage sets in sooner than with either disorder alone.

Why insomnia plus sleep apnea strains the heart
During consolidated sleep, the cardiovascular system shifts into a lower-gear mode: blood pressure dips, heart rate slows, and vessels repair microscopic damage. With chronic Sleep Deprivation from insomnia, those restorative phases shrink. When Sleep Apnea is added, each pause in breathing triggers a spike in blood pressure and stress hormones.
Over months and years, this pattern reshapes physiology. The combination fuels chronic inflammation, stiffens arteries, and disrupts metabolic regulation. Similar mechanisms are described in recent cardio‑sleep studies available in journals like the Journal of the American Heart Association and in analyses hosted on platforms such as PubMed Central, all pointing to a shared final pathway: higher Cardiovascular Risk and earlier onset of Chronic Conditions.
What the veteran study actually found about heart disease
The Yale researchers examined veterans at an age where many still feel “too young” for cardiac trouble. Yet COMISA already correlated with a steeper trajectory toward hypertension and other Risk Factors for Heart Disease. Compared with veterans without sleep issues, those with both insomnia and apnea showed significantly higher odds of elevated blood pressure and doctor-diagnosed cardiovascular disease.
These findings echo previous results in older adults and now extend concern to younger, often active populations. For clinicians, that means a 40‑year‑old veteran with persistent insomnia and loud snoring is no longer just “tired”; that person belongs in a high‑risk bracket, similar to someone with early diabetes or longstanding smoking.
The hidden cost of treating only one sleep problem
In real life, many patients resemble Mark, a fictional 45‑year‑old veteran who struggles to fall asleep, wakes repeatedly, and has been told he “probably” snores. His primary care team prescribes medication for insomnia but delays a sleep study for apnea. Months later, his blood pressure climbs, and lifestyle advice alone fails to control it.
This scenario illustrates why the study’s authors argue that ignoring one part of the problem weakens overall care. When insomnia is treated in isolation, undiagnosed apnea can continue to drive nightly oxygen drops. When only apnea is addressed, unresolved insomnia leaves the nervous system in a state of hyperarousal, perpetuating elevated Cardiovascular Risk despite CPAP adherence.
Turning sleep into a strategic tool against chronic disease
Cardiology has long focused on cholesterol, blood pressure, and smoking. The Yale work, supported by other studies accessible through resources like the recent veteran-focused coverage, suggests that structured evaluation of Sleep Disorders belongs on the same checklist. Clinicians are encouraged to ask targeted questions about both insomnia symptoms and signs of apnea during routine cardiovascular visits.
For patients, this reframing can be empowering. Rather than viewing poor sleep as a side effect of stress or aging, you can treat it as a modifiable lever, much like diet or exercise. Many people now integrate sleep tracking, cognitive behavioral therapy for insomnia, and apnea testing into a broader heart‑health plan, alongside measures discussed in other research on systemic inflammation and aging, such as the analyses of immune regulation described in recent inflammation research reports.
Practical steps to lower sleep‑related cardiovascular risk
Several concrete actions help transform this science into daily practice. Even before a formal diagnosis, you can start to adjust routines and prepare for medical evaluation. The key is to act early, when damage is still reversible and before Chronic Conditions fully establish.
- Screen systematically for both insomnia symptoms (difficulty falling asleep, frequent awakenings) and apnea signs (snoring, gasping, morning headaches).
- Request a sleep study if you have daytime sleepiness, high blood pressure, or bed partner reports of breathing pauses.
- Prioritize sleep timing by stabilizing bed and wake times, limiting late caffeine, and protecting a 7–9 hour sleep window.
- Combine therapies, such as CPAP or oral appliances for apnea with cognitive behavioral therapy for insomnia.
- Monitor blood pressure at home once sleep treatment begins to track improvements in Health Impact.
These steps turn sleep from a background complaint into a measurable component of cardiovascular prevention, much like controlling weight or managing blood sugar.
How do I know if I have both insomnia and sleep apnea?
Persistent trouble falling or staying asleep suggests Insomnia, while loud snoring, gasping, and unrefreshing sleep point to Sleep Apnea. When these signs coexist, especially with daytime fatigue or high blood pressure, a formal sleep evaluation with overnight monitoring is strongly recommended.
Does treating sleep apnea alone reduce heart disease risk enough?
Treating Sleep Apnea with CPAP or another device clearly lowers Cardiovascular Risk, but the new data show that leaving insomnia untreated can maintain elevated stress and blood pressure. Combining apnea therapy with evidence-based insomnia treatment offers a stronger protective effect against Heart Disease.
Can lifestyle changes fix COMISA without medical help?
Improving sleep hygiene, reducing alcohol, and maintaining a healthy weight can ease symptoms and other Risk Factors. However, COMISA involves physiological changes that usually require professional assessment, such as a sleep study and targeted therapies, to significantly reduce long-term Health Impact.
Are younger adults really at risk from combined sleep disorders?
Breathtaking Maps Unveil DNA’s Architecture Before Life Begins
More Additional Dog Breeds Face Respiratory Risks
Yes. The veteran study focused on relatively young and middle-aged adults and still found higher rates of hypertension and cardiovascular disease with COMISA. Early Sleep Deprivation and oxygen drops create a long runway for damage, making prompt diagnosis and treatment particularly valuable.
How fast can heart health improve after treating sleep problems?
Some patients see blood pressure and daytime alertness improve within weeks of consistent apnea and insomnia treatment. Structural vascular changes take longer, yet research indicates that addressing combined Sleep Disorders early can slow progression toward Chronic Conditions and lower lifetime Cardiovascular Risk.