Show summary Hide summary
- Serotonin from gut bacteria: a new IBS frontier
- The two bacteria that manufacture serotonin together
- What this means for irritable bowel syndrome patients
- How you could support a serotonin-friendly microbiome
- How are serotonin-producing gut bacteria different from regular probiotics?
- Can these bacteria cure irritable bowel syndrome?
- Are serotonin-focused probiotics already available to buy?
- How does this research change current IBS treatment strategies?
- What should someone with IBS discuss with their doctor now?
You know IBS is more than “just a sensitive stomach”, but what if part of the solution lived quietly in your gut, making Serotonin on demand? New research shows specific Gut Bacteria act like tiny pharmacies, reshaping the Gut-Brain Axis and opening real Treatment prospects.
Serotonin from gut bacteria: a new IBS frontier
Irritable Bowel Syndrome (IBS) disrupts Digestive Health with pain, bloating, constipation, diarrhea, and a constant fear of flare-ups. Women are affected more often, yet many patients still leave consultations with vague answers and trial‑and‑error medications.
Researchers from the University of Gothenburg have now mapped how particular microbes in the Microbiome manufacture Serotonin, the same molecule known for mood but produced mostly in the intestine. Their work, highlighted in sources such as recent coverage on serotonin-producing bacteria, reframes IBS as a disorder of microbial chemistry rather than only “nervous bowels”.
A Serendipitous Lab Error at Cambridge Uncovers a Groundbreaking Technique to Transform Drug Molecules
AI-Powered Toys Are Here to Stay, But Their Safety Remains Uncertain
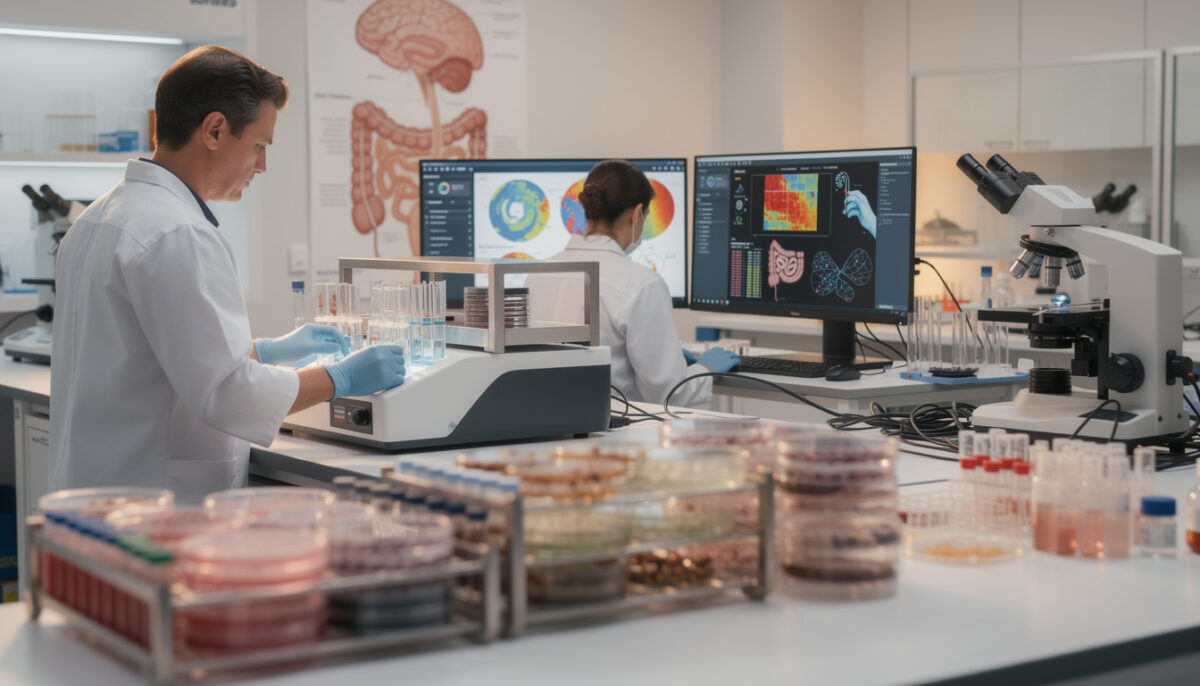
How gut-made serotonin shapes bowel movements
More than 90% of the body’s Serotonin is generated in the intestine, not the brain. Specialized enterochromaffin cells convert tryptophan into Serotonin, which then signals through the enteric nervous system, sometimes called the “second brain”.
When this signaling drifts out of balance, bowel motility speeds up or slows down. Diarrhea‑predominant IBS links to exaggerated signaling, while constipation‑predominant forms seem tied to sluggish Serotonin dynamics. This is where specific Gut Bacteria suddenly enter the picture. Revolutionary approaches targeting specific bacteria may pave the way for breakthrough treatments in related digestive disorders.
The two bacteria that manufacture serotonin together
In experiments reported in Cell Reports, scientists identified a duet of human Gut Bacteria able to synthesize bioactive Serotonin directly in the colon: Limosilactobacillus mucosae and Ligilactobacillus ruminis. Alone, they are interesting; together, they behave like a biochemical production line.
The microbes decarboxylate 5‑hydroxytryptophan, a Serotonin precursor, effectively finishing the last step usually attributed only to host cells. This finding, also discussed in recent microbiome research reports, demonstrates that the Microbiome does not just nudge host cells; it can create active Neurotransmitters itself.
From germ-free mice to restored intestinal motility
To understand impact rather than just chemistry, researchers turned to germ‑free mice lacking normal Serotonin levels. These animals showed reduced colonic neurons and slowed transit, mirroring severe constipation patterns seen in some IBS cases.
After introducing the L. mucosae and L. ruminis consortium, fecal Serotonin rose, colonic neuronal density increased, and transit time normalized. In other words, adding the bacteria rebooted the gut’s neural hardware and motility, a powerful proof of concept for future IBS Treatment designs.
What this means for irritable bowel syndrome patients
The next question naturally concerns humans. When researchers compared stool samples, individuals with Irritable Bowel Syndrome showed lower levels of L. mucosae than healthy controls. That species carries the enzyme machinery required for Serotonin synthesis.
This imbalance supports what many clinicians already suspect: IBS is not only psychological stress or diet, but a disturbed Microbiome modulating the Gut-Brain Axis. Reduced Serotonin‑producing Gut Bacteria might translate into altered signaling, pain sensitivity, and unpredictable bowel habits.
From generic probiotics to targeted microbial therapy
Generic Probiotics shelves are crowded, yet most products were not designed around Neurotransmitters or IBS mechanisms. The Gothenburg work pushes toward next‑generation formulations based on specific strains with documented Serotonin activity and measurable effects on motility. For further reading on cellular molecular mechanisms, you may find insight in reviewing nuclear cell metabolism processes.
Future strategies could combine L. mucosae and L. ruminis with prebiotics that feed them, or personalized blends guided by stool sequencing. For a patient like “Sarah,” a 32‑year‑old with mixed‑type IBS, this may eventually mean tailored microbial capsules instead of rotating laxatives and antispasmodics.
How you could support a serotonin-friendly microbiome
While these Serotonin‑producing strains are not yet standard therapy, current knowledge around the Microbiome and Digestive Health points toward several practical levers you may already use alongside medical care.
- Fiber variety: rotating whole grains, legumes, fruits, and vegetables offers substrates for diverse Gut Bacteria, supporting balanced fermentation and signaling.
- Fermented foods: yogurt with live cultures, kefir, and sauerkraut introduce lactic acid bacteria, distant cousins of the strains studied for Serotonin production.
- Stress management: breathing exercises, cognitive‑behavioral approaches, and regular movement modulate the Gut-Brain Axis and can reduce visceral hypersensitivity.
- Medication review: some drugs alter microbial communities or Serotonin pathways; discussing options with a clinician avoids unwanted interference.
- Data tracking: food and symptom logs help map personal triggers and may one day integrate with Microbiome profiling tools.
These steps do not replace medical Treatment, yet they position your gut environment to benefit sooner from targeted Probiotics once strain‑specific products for IBS reach routine practice.
How are serotonin-producing gut bacteria different from regular probiotics?
Most conventional probiotics are selected for general benefits such as supporting digestion or immunity. Serotonin-producing Gut Bacteria, like Limosilactobacillus mucosae and Ligilactobacillus ruminis, are identified because they synthesize bioactive Serotonin and influence the Gut-Brain Axis. Future products based on these strains would be designed specifically for motility and IBS-related signaling, rather than broad, non-targeted support.
Can these bacteria cure irritable bowel syndrome?
Current data from animal models and human stool analyses are promising, but they do not amount to a cure yet. The findings suggest these microbes could become one pillar of Treatment for Irritable Bowel Syndrome, alongside diet, stress management, and medication when needed. Clinical trials in humans must still confirm efficacy, appropriate doses, and long-term safety before they can be used routinely.
Are serotonin-focused probiotics already available to buy?
As of now, no widely available product is marketed explicitly as a Serotonin-producing consortium for IBS based on the exact strains studied. Some supplements contain related lactic acid bacteria, but their capacity to generate Neurotransmitters is rarely documented. If you consider Probiotics, discuss brands and evidence with a healthcare professional rather than self-prescribing solely based on marketing claims.
How does this research change current IBS treatment strategies?
Unveiling the Unexpected Tactics Bacteria Use to Move Without Propellers
Depression Could Begin with Cellular Energy Deficits in the Brain
These findings strengthen the view of IBS as a disorder involving the Microbiome and Neurotransmitters, not only stress or diet. They encourage clinicians to think about microbial composition, stool tests in some cases, and future strain-specific therapies. Over time, Treatment could shift from symptomatic control toward reprogramming gut signaling using targeted microbes that restore Serotonin balance and intestinal motility.
What should someone with IBS discuss with their doctor now?
You can ask how your current symptoms relate to the Gut-Brain Axis and Serotonin, whether your medications interact with these pathways, and if any evidence-based Probiotics fit your profile. Bringing research articles, such as recent work on Serotonin-producing Gut Bacteria and IBS, can open a collaborative conversation on future options while you optimize today’s management plan.


