Show summary Hide summary
- How AI Spots the Invisible: The Game-Changer in Skin Cancer Detection
- The Promise—and Peril—of AI Overdiagnosis: Not Every Spot is Cancer
- What AI Sees—And What It Still Can’t: The Hidden Limitations of Smart Detection
- From Clinic to Pocket: Will Your Next Checkup Start with a Selfie?
- What Happens When AI Gets It Wrong? Uncomfortable Consequences and Future Dilemmas
- The Next Warning Your Doctor Might Miss: Will You Trust a Machine With Your Skin?
- FAQ
Imagine snapping a photo of a mole with your phone and getting an instant warning about your risk for skin cancer—without ever setting foot in a specialist’s office. This is no longer a sci-fi promise. AI identifies early risk patterns for skin cancer after analyzing millions of images, and the results are so precise that researchers are questioning whether digital detection could become our first line of defense. But as artificial intelligence redefines early screening, it also brings a wave of uneasy questions about trust, accuracy, and the limits of machine insight.
Why does this matter now? Skin cancer rates are rising around the world, and early intervention is critical. The ability to spot tiny changes—details invisible to even the sharpest human eye—could save lives and ease the burden on overloaded clinics. Yet as algorithms move from the research lab to the palm of your hand, we’re forced to ask: can you trust a machine with your skin health, or is the promise of AI-fueled vigilance hiding risks we’re only beginning to see?
How AI Spots the Invisible: The Game-Changer in Skin Cancer Detection
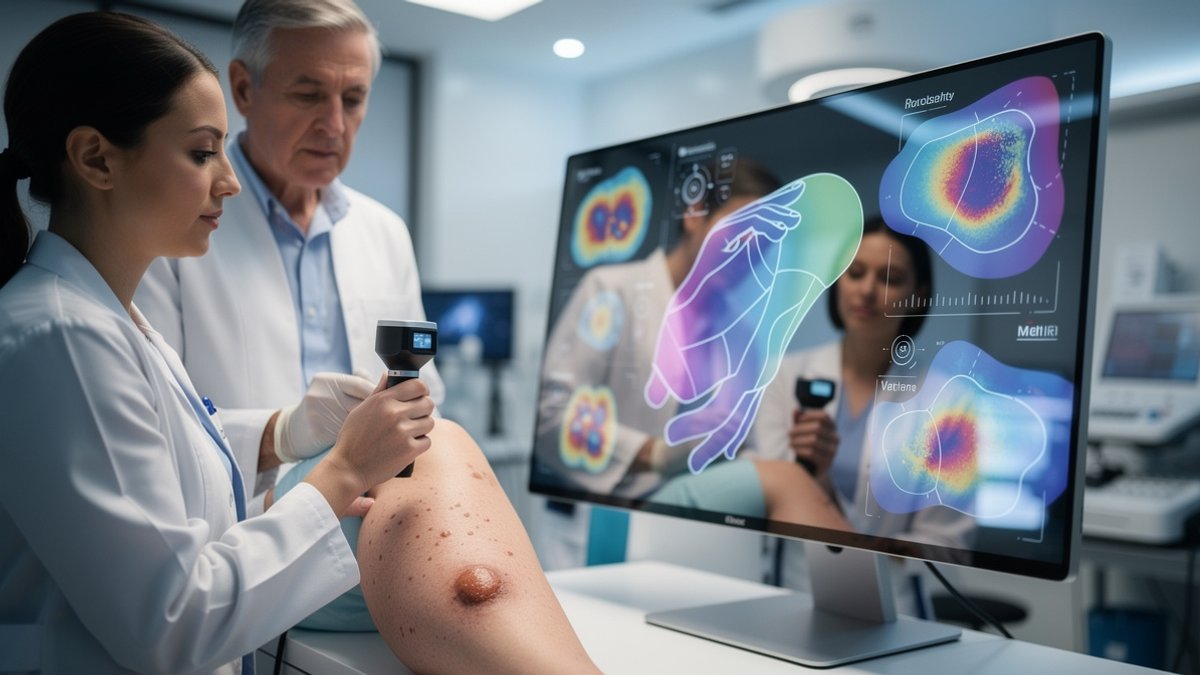
The future of skin cancer diagnosis might come down to a few milliseconds of machine learning calculations. Advanced algorithms are now trained to recognize diagnostic patterns in thousands of skin lesion images, unlocking subtle clues that even seasoned dermatologists can miss. What once required a magnified lens and years of clinical experience could soon be within reach of anyone with a smartphone camera.
The Surprising Reason Productivity Swings So Sharply—And Why It Might Have Nothing to Do With Motivation or Discipline
95% of people already carry this silent virus—but a new scientific discovery may finally reveal how to stop it for good
- At the core of early detection technology is the ability to identify microscopic shifts in color gradation, border irregularity, or textural nuance—changes too faint for the human eye.
- For example, an AI-assisted app may flag a seemingly ordinary freckle as a concern, based on complex patterns it has learned from millions of cases.
- This isn’t science fiction: recent studies show that machine learning models can sometimes match, or occasionally exceed, expert-level accuracy in skin lesion analysis.
But as AI identifies early risk patterns for skin cancer with unprecedented speed, new layers of doubt emerge. Can these systems avoid missing rare cancer presentations? Will the public trust an algorithm more than a dermatologist’s eye, or will false alarms erode confidence in the technology altogether? As diagnostic power migrates from clinics to pockets, the promise of catching skin cancer early must confront the gray zones of accuracy versus overdiagnosis. Suddenly, the quest to save lives becomes as much about building trust as it is about perfecting algorithms.
The Promise—and Peril—of AI Overdiagnosis: Not Every Spot is Cancer
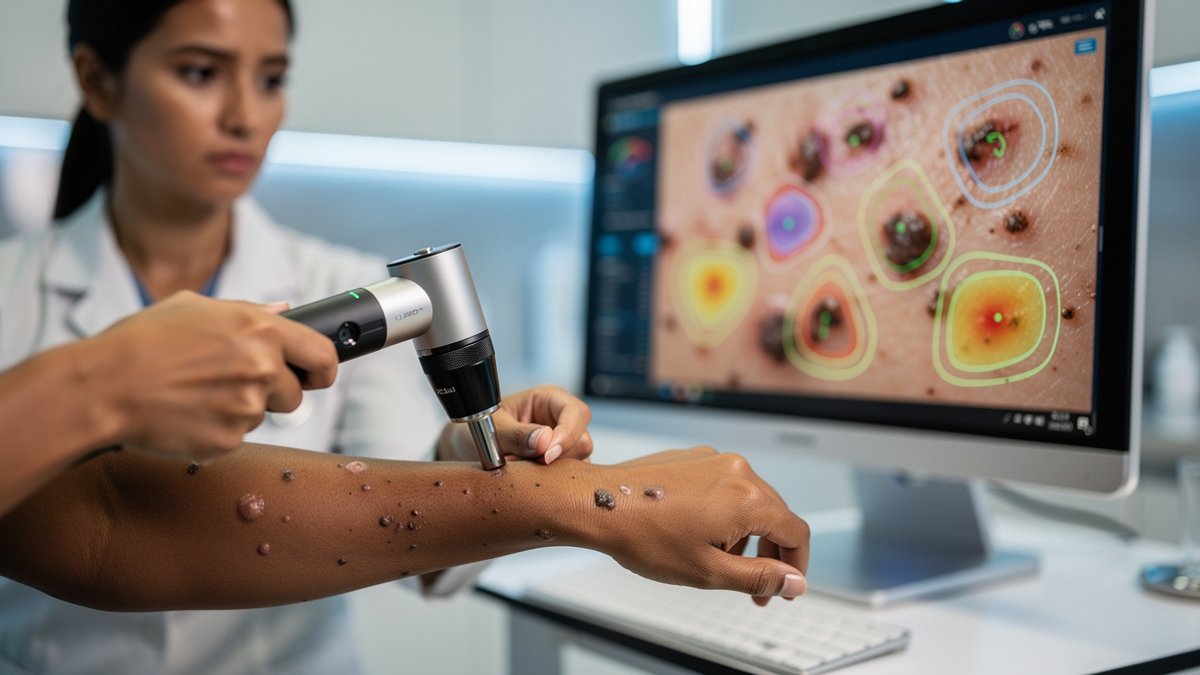
- As AI identifies early risk patterns for skin cancer at unprecedented speed, a new dilemma surfaces: machines often ring alarm bells for spots that would never have posed a threat.
- False positives—instances where harmless moles are flagged as dangerous—can set off a cascade of biopsies, anxiety, and unnecessary treatments.
- For patients, this means the promise of early detection is shadowed by the risk of overdiagnosis and the emotional toll of fearing something that may not exist.
Balancing predictive accuracy with real-world clinical risk assessment is now the field’s central challenge. A system ultra-sensitive to cancer markers can flood clinics with cases that need no intervention, straining resources and trust alike. The tension between catching every dangerous change and misdiagnosis—seeing cancer where there is none—remains a puzzle only rigorous testing and transparent thresholds can solve. For more on paradigm-defining scientific validation, see our feature on gravitational wave detection.
What AI Sees—And What It Still Can’t: The Hidden Limitations of Smart Detection
Even the smartest detection models can miss what’s right in front of them. Algorithm bias remains a stubborn flaw, especially when data diversity lags behind medical reality. If an AI system is mostly trained on images of lighter skin tones, its sensitivity often plummets for patients with darker complexions or atypical lesions. The promise of skin tone inclusivity is still a work in progress.
Rare skin cancers pose their own challenge. With fewer available images, these dangerous outliers often slip beneath the radar of even the most sophisticated algorithms. Such model limitations are not theoretical—they carry real consequences for diagnosis and care. As AI identifies early risk patterns for skin cancer, uneven detection may reinforce healthcare disparities rather than erase them. The path toward universal, trustworthy smart detection is far from clear, and every patient brings a new unknown into focus.
From Clinic to Pocket: Will Your Next Checkup Start with a Selfie?
- Your phone may soon become your first line of defense. Developers are rapidly adapting lab-based AI tools for mobile health devices, letting people analyze suspicious spots through teledermatology apps without setting foot in a clinic.
- This shift promises unprecedented patient empowerment and could shrink the distance between specialist and sufferer—especially in rural areas or for those reluctant to visit a dermatologist.
- For another example of innovation outside the clinic, see our analysis of nasal spray shows promise in flu prevention.
Yet democratizing access comes with hard questions. Easy diagnoses on a smartphone demand serious consideration of digital health privacy, as sensitive images and health data travel far beyond the doctor’s office. If patients start self-screening, who is truly responsible for interpreting results—and ensuring follow-up? The rise of AI-powered skin checks on personal devices hints at a future where care is more accessible, but the boundary between convenience and caution grows blurrier by the day.
What Happens When AI Gets It Wrong? Uncomfortable Consequences and Future Dilemmas
When algorithms miss a cancerous lesion or flag a harmless spot as dangerous, the outcome is not just personal—it can shape the future of medical liability itself. Diagnostic error is nothing new in medicine, but when a machine gets it wrong, who takes responsibility? Patients and physicians are left navigating new fault lines: Is the designer of the software accountable, or the clinician who followed its suggestion?
AI trust becomes fragile with every misstep. A mistaken scan could lead to unnecessary biopsies, spiraling anxiety, or, far worse, a missed window for life-saving treatment. Regulators, insurers, and hospital systems are already grappling with what robust clinical oversight should look like in an era where decisions may start on a smartphone. The hope is real, but so are the stakes—and the answers remain as unsettled as ever. Explore how regulatory uncertainty affects other disciplines in our summary of the top must read popular science releases.
The Next Warning Your Doctor Might Miss: Will You Trust a Machine With Your Skin?
We are nearing a crossroads in the future of screening for skin cancer. Digital diagnosis tools could soon alert you to signs your doctor might overlook, making your phone—not your physician—the first responder. Yet for many, trusting a machine with such intimate, life-altering news feels deeply unsettling.
Patient decision-making is entering unfamiliar territory. Rapid advances clash with lingering skepticism, and regulatory challenges are slowing the path from lab to clinic. Who certifies the algorithms? What if one app flags a lesion and another dismisses it? Even as AI identifies early risk patterns for skin cancer, the human urge for a second opinion remains powerful.
So the dilemma is immediate: Should you risk waiting weeks for an in-person appointment, or act when a silicon sentinel turns cautious? Like it or not, the front line of cancer detection may soon be in your hand. How you respond could shape what “caught early” really means.
FAQ
How accurate is AI skin cancer detection compared to a dermatologist?
Recent studies suggest that AI skin cancer detection can reach or even exceed the accuracy of experienced dermatologists in identifying certain types of lesions. However, AI tools may still struggle with rare or unusual skin presentations, so human oversight remains important.
Can I rely solely on an AI app to monitor my moles and skin changes?
While AI apps can provide useful early warnings, they should not replace professional medical advice. If an app flags a concern, it’s always best to consult with a dermatologist for a thorough evaluation.
Are there privacy risks when using AI skin cancer detection apps on my mobile device?
Stanford’s ‘Natural Ozempic’ Discovery: Is the Side-Effect-Free Weight Loss Hype Missing a Critical Risk?
Scientists Uncover Powerful Spice Combination That Amplifies Anti-Inflammatory Effects by 100 Times
Some AI skin cancer detection apps require uploading images of your skin, which could raise privacy concerns if not managed securely. Always use apps from reputable providers and review their privacy policies before sharing personal health data.
What happens if an AI system gives a false positive or false negative result?
AI systems can occasionally misclassify skin lesions, leading to unnecessary worry or, less often, missed diagnoses. This is why AI results should be used as a prompt for seeking further professional assessment, not as a standalone decision.